Chronic venous ulcers are the most serious and intractable complication of chronic venous insufficiency (CVI) in the lower extremities, with a total population incidence of 0.4-1.3%. Venous ulcers (clinical grades C5 and C6) are reported to be present in about 12-14% of CVI patients and are associated with distal venous hypertension.
In the past, CVI and its accompanying venous hypertension have long been considered as post-thrombotic syndrome due to the regurgitation and / or obstruction of the deep venous system secondary to deep venous thrombosis. With the widespread use of color Doppler ultrasound technology, Color Doppler provides accurate anatomical and functional data on all venous system regurgitation and obstruction in the CVI, giving people a deeper understanding of the pathogenesis of CVI. For example: the formation of venous leg ulcers, in addition to the surrounding tissue, primary valve insufficiency is an important factor, and superficial veins and traffic veins dysfunction, simple or combined, can also cause ulcer formation.
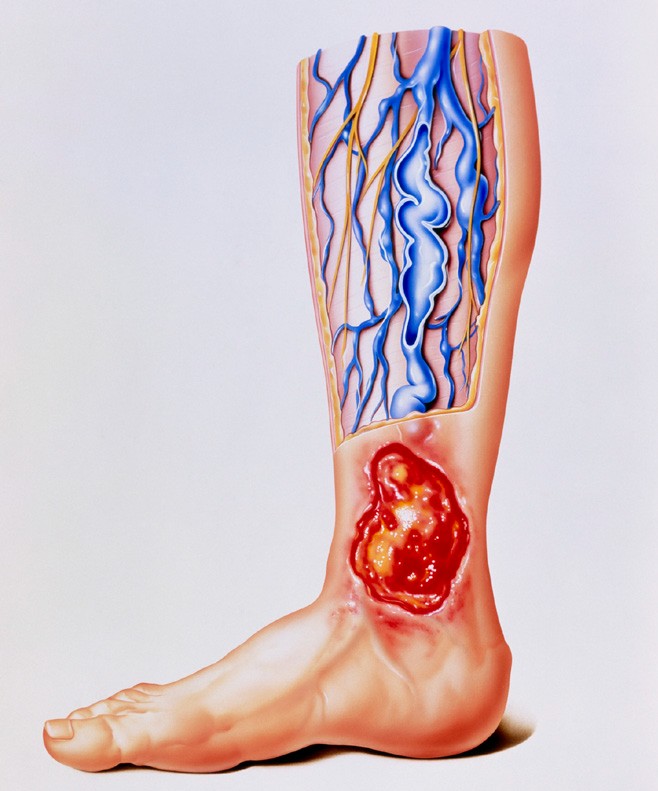
The main hemodynamic mechanism of venous ulcer formation is regurgitation, venous reflux obstruction, or a combination of the two, and dysfunction of the calf muscle is also associated with it. Recent studies have shown that inadequate calf muscle dysfunction significantly inhibits ulcer healing.
1 Venous return and venous hypertension
Various causes of lower extremity venous valve insufficiency, can produce abnormal venous reflux, leading to elevated venous pressure. It has been recognized that continuous venous hypertension can cause local blood circulation and tissue absorption disorders, accumulation of metabolites, tissue malnutrition, lower extremity edema and skin nutrition changes, is the main cause of venous ulcers. Cause venous valve insufficiency for many reasons, can be divided into primary and secondary. Among them, the incidence of primary deep venous valve insufficiency is the highest, while the secondary is mainly the sequelae of deep venous thrombosis.
Venous regurgitation is CVI and is also the most common mechanism of venous ulcers. Thirteen clinical studies that included 1,249 limbs of venous ulcers clearly demonstrated venous regurgitation in 92% (1153) of the limbs. Only two reports reported a lower prevalence of venous reflux, 71% and 83%, respectively, but the two reported only superficial and deep venous systems without imaging of veins. All other reported venous reflux rates were over 90%. The reflux of 45% of the limbs is confined to the superficial venous system or to both the superficial and the communicating veins, and the deep venous system of these limbs is normal. This is a meaningful finding because it shows that when venous ulcers are caused solely by superficial venous system and traffic venous insufficiency. Surgical treatment can improve ulcer healing rate of 90%, and has good long-term efficacy. One group of studies showed that the median time required for ulcer healing after superficial vein surgery was 18 weeks, with ulcer healing rates of 57%, 74% and 82% at 6, 12 and 18 months, respectively. More intriguing than the overall rate of healing, the rate of ulcer recurrence within 2 years after superficial vein surgery was less than 4% with compression alone. The study also shows that these ulcer limbs involving the superficial venous system up to 88%, indicating that superficial venous system insufficiency plays an important role in the formation of venous ulcers, which is associated with the presence of gravity hydrostatic regurgitation in the superficial venous system .
Whether primary or secondary venous insufficiency, due to valvular dysfunction and the formation of gravity reflux in the calf muscle contraction after the early filling of the venous pool. Under normal conditions, however, when muscle contractions, superficial and deep venous system pressure are increased, when the muscles are relaxed, the pressure is lower, lower than the pressure of the muscular plexus. At this point, a well-functioning valve serves as a protective barrier against backflow of blood in the venous system. During muscle contraction, the internal pressure of the muscular and deep venous systems is higher than that of the superficial venous system. During relaxation of the muscles, the internal pressure of the deep venous system drops below the internal pressure of the superficial venous system. When the valve is impaired, the re-filling time of the calf intramuscular vein after muscle contractions is shortened due to venous regurgitation, thereby involving the progressive and progressive increase of intramuscular venous pressure, which is called ambulatory venous hypertention. . It arises from the weight of the blood column from the right atrium and is transmitted through the flapless pelvic and pelvic veins to the impaired lower extremity veins. Peripheral venous valvular dysfunction may be primary or secondary, but the dysfunctional valve has the same hemodynamic effects – distal venous hypertension, which also results in telangiectasia, plasma, plasma proteins and Red blood cell leakage increased.
Leave a Reply